Stem Cell Therapy for Joint Pain in Phuket — Lyfe Medical Wellness
Physician-supervised UC-MSC stem cell injections for knee pain, joint degeneration, cartilage repair and sports injuries — at Lyfe Medical Wellness, Phuket.
What Is Stem Cell Therapy for Joint Pain?
Stem cell therapy for joint pain is a targeted regenerative medicine intervention — delivering a concentrated dose of umbilical cord mesenchymal stem cells (UC-MSCs) directly into a damaged or degenerated joint to support structural repair, reduce inflammation and restore functional mobility.
The fundamental challenge of joint degeneration — particularly osteoarthritis — is that cartilage has extremely limited capacity for self-repair. Unlike most body tissues, articular cartilage receives minimal blood supply and contains very few resident stem cells. Once lost, it does not regenerate naturally. Conventional medicine manages the symptoms — pain relief, physiotherapy, steroid injections — but does not address the underlying structural decline.
Stem cell therapy works differently. UC-MSCs are not passive cells — they are active biological agents. When delivered into the joint environment, they release growth factors (including TGF-beta, PDGF and IGF), modulate the inflammatory immune response and stimulate the resident cells of the joint to support repair and regeneration.
What Joint Conditions Does Stem Cell Therapy Address?
What Joint Conditions Does Stem Cell Therapy Address?
HOW IT IS DELIVERED
How Is Stem Cell Joint Therapy Administered at Lyfe Medical Wellness?
The Cells
UC-MSCs are used — the same quality-tested, ethically sourced cells used in our systemic rejuvenation programme. Each batch is tested for sterility, viability and potency before clinical use.
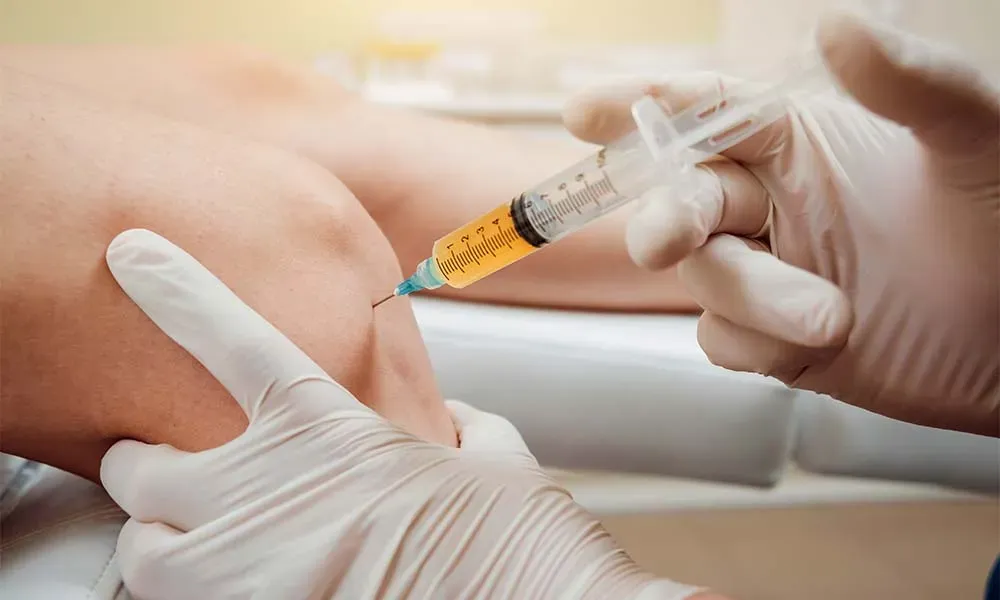
The Injection
Cells are injected directly into the target joint — typically the knee — using anatomically landmarked injection technique. This is a clinically precise approach based on the physician’s anatomical expertise and knowledge of joint structures. The full session including preparation takes 60 to 90 minutes.
Local vs Systemic
Unlike the rejuvenation programme (IV infusion for systemic effect), joint stem cell therapy is a local procedure — cells are concentrated at the site of damage. In some cases, a combination of local injection and a lower-dose systemic IV may be recommended. Your physician will advise.
Programme Structure
Most patients begin with a single injection session to assess response. Depending on severity and response, a second injection at 3 to 6 months may be recommended. Your physician designs the programme individually — there is no fixed protocol.
UNDERSTANDING YOUR OPTIONS
Stem Cell Therapy vs Conventional Joint Pain Treatments
|
Treatment |
What It Does and Its Limitations |
|---|---|
| Pain medication (NSAIDs) | Masks pain without addressing the biological cause. Provides temporary relief; does not slow joint degeneration. |
| Steroid injections | Reduces inflammation temporarily. Effects are short-lived (weeks to months). Repeated use may damage cartilage over time. |
| Physiotherapy | Supports muscle strength and joint stability. Valuable but does not address cartilage loss or joint inflammation. |
| Hyaluronic acid injections |
Lubricates the joint. Short-term pain relief in some patients. Does not regenerate cartilage. |
| PRP therapy | Uses the patient’s own growth factors. Can reduce inflammation and support repair. Good for mild to moderate OA. Can be used alongside stem cells. |
| Stem cell therapy (UC-MSC) | Targets the biological root: reduces inflammation, supports cartilage matrix repair, delivers growth factors. Effects develop over months. Non-surgical with minimal downtime. |
| Joint replacement surgery | Definitive for end-stage OA. Major surgery with significant recovery. Many patients use stem cell therapy to delay or avoid this outcome. |
WHO IS THIS FOR?
Who Is a Good Candidate for Stem Cell Joint Therapy?
Stem cell joint therapy is not appropriate for patients with end-stage joint destruction, active joint infection, or certain autoimmune conditions. A thorough medical assessment — including review of any available imaging — is required before any programme begins.
Your Stem Cell Joint Therapy Journey at Lyfe Medical Wellness
Combining Stem Cell Therapy with Other Joint Treatments
Is Stem Cell Joint Therapy Safe?
UC-MSC joint injections have a well-documented safety profile in clinical orthopaedic settings when performed by a trained physician using quality-tested cells. Common post-treatment responses include:
Stem Cell Joint Therapy — Frequently Asked Questions
“Stem cell therapy is a medical decision — not a wellness product. Every patient who comes to us deserves a physician’s assessment, not a menu of pre-packaged treatments.”
At Lyfe Medical Wellness, we believe the most important thing we can offer a patient is honest, personalised medical guidance — before any treatment begins.

RELATED TREATMENTS
Explore Other Regenerative Treatments

Ready to Start Your Treatment Journey?
Our team will respond within 24 hours. Initial consultation with no obligation.
Phone
+66 94 926 3269
info@lyfemedical.com
Book Your Consultation
Fill the form and we will contact you within 24 hours.
